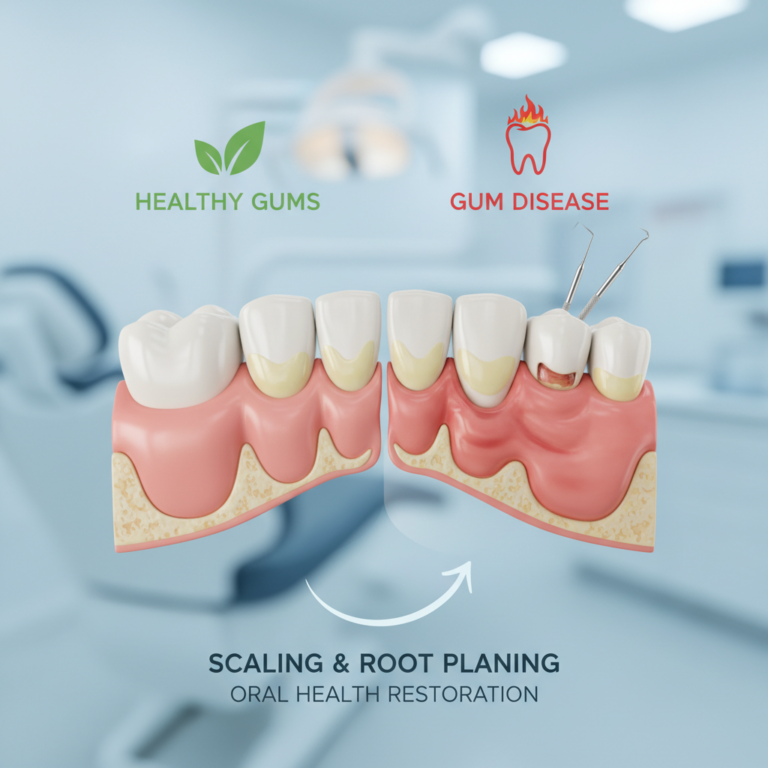
Understanding how gum disease is treated
If you are noticing bleeding when you brush, tender gums, or persistent bad breath, you might be wondering, “how is gum disease treated, and how serious is this?” Gum disease, also called periodontal disease, ranges from mild gingivitis to advanced periodontitis, and treatment depends heavily on how early you catch it and how involved the supporting bone and gums have become.
Your dentist or periodontist will focus on two main goals. First, they will remove the plaque and tartar that caused the infection in the first place. Second, they will create conditions that allow your gums to heal and make it harder for bacteria to cause damage in the future. In many cases, this means moving from routine cleanings to a deeper procedure called scaling and root planing, sometimes followed by more advanced therapies if the disease is severe.
Early versus advanced gum disease
Gum disease progresses in stages, and understanding where you are on that spectrum helps clarify which treatments you need and why.
Early gum disease: gingivitis
In the earliest stage, plaque accumulates along the gumline and irritates the gums. You might notice:
- Bleeding when you brush or floss
- Red or swollen gums
- Mild tenderness
- Occasional bad breath
At this point, the bone and deeper supporting tissues are usually not yet damaged. According to the Cleveland Clinic, early-stage gum disease can often be reversed with regular professional cleanings and consistent home care, including brushing two to three times a day, flossing daily, and routine dental exams [1].
If you are in this stage, your dentist may focus on early stage gum disease treatment and repeated cleanings instead of deep periodontal therapy. Good habits at home can be enough to restore your gum health before permanent damage occurs.
Advanced gum disease: periodontitis
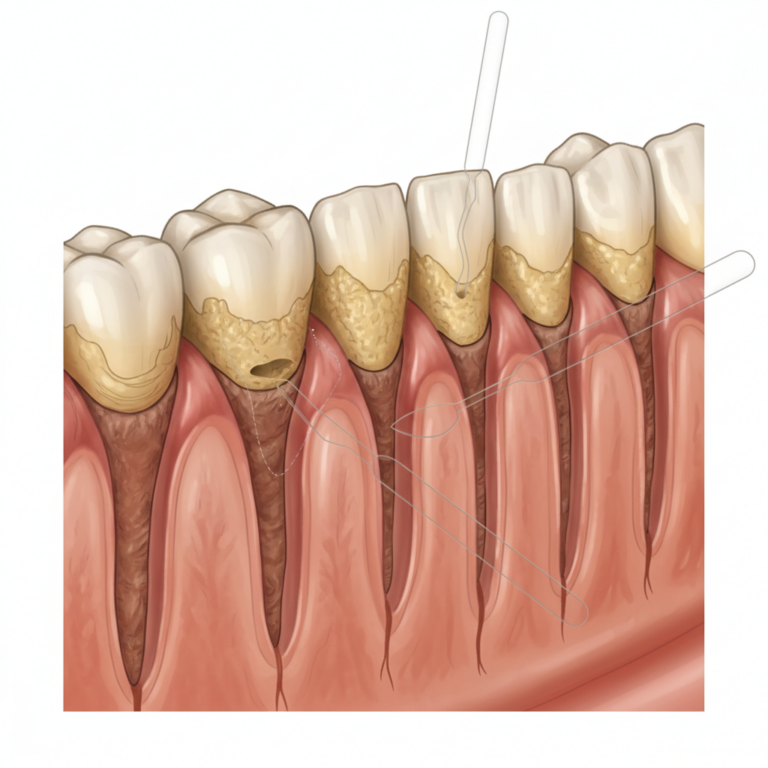
If plaque is not removed, it hardens into tartar and begins to creep under the gumline. This leads to periodontitis, a more serious form of gum disease that can destroy bone and connective tissue.
Signs often include:
- Gums pulling away from teeth, creating pockets
- Persistent bad breath
- Teeth that feel loose or shift in position
- Gum recession and longer-looking teeth
- Bleeding and swelling that do not improve with routine cleaning
The Mayo Clinic notes that treatment for periodontitis is designed to thoroughly clean the pockets around teeth and prevent further damage to bone and gums. Lifestyle factors such as stopping tobacco use and managing overall health conditions are also critical to success [2].
Once you reach this stage, routine cleanings are not enough. Deep cleaning with scaling and root planing and, in some cases, surgery become necessary to control the infection and protect your teeth.
How your dentist evaluates gum disease
Before deciding how your gum disease is treated, your dental team will perform a periodontal evaluation. This process helps determine whether you simply need a routine cleaning or whether you need a deep cleaning or even surgery.
You can expect your provider to:
- Review your medical history and risk factors, such as smoking, diabetes, or medications that affect your gums
- Measure the depth of gum pockets around each tooth with a small probe
- Check for gum recession and areas of bleeding
- Take X-rays to look for bone loss
Pocket depths of 1 to 3 millimeters are considered healthy. When pockets reach 4 millimeters or more and X-rays show bone loss, you are moving into periodontitis, and scaling and root planing is often recommended.
If you are unsure whether your symptoms justify this deeper treatment, you can review the signs you need scaling and root planing and then discuss your questions with your dentist.
Nonsurgical gum disease treatments
Nonsurgical periodontal therapy aims to control infection and stabilize your gums without incisions or stitches. The specific approach depends on how advanced your condition is.
Routine dental cleaning and improved home care
For early gingivitis, your dentist will usually start with:
- Professional cleaning to remove plaque and tartar above the gumline
- Polishing to smooth enamel surfaces
- Coaching on brushing and flossing technique
Cleveland Clinic notes that early gingivitis can be reversed with regular dental cleaning and diligent oral hygiene, which supports your gums before deeper tissues are damaged [1].
This is the stage where consistent daily care at home has the greatest impact. If you want to know more about whether gum disease can be reversed, the answer depends greatly on catching it at this early point.
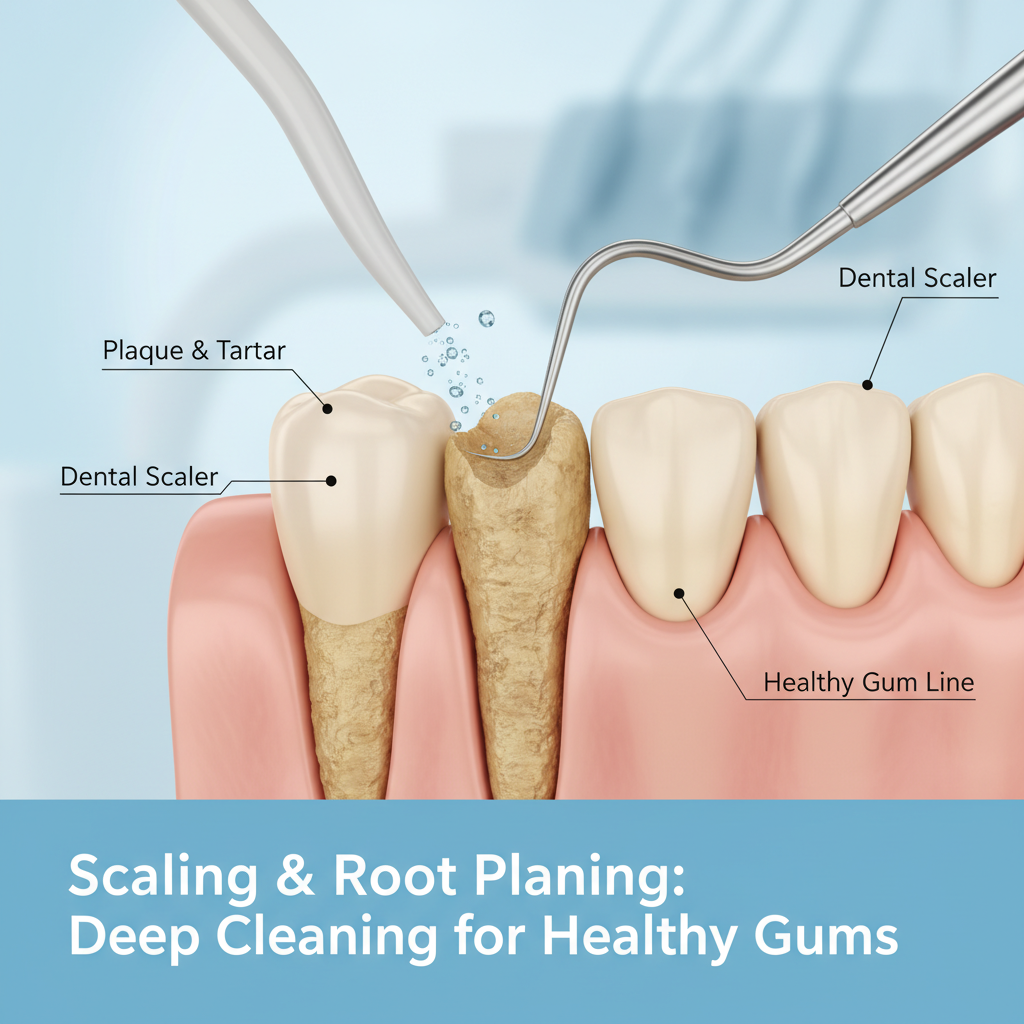
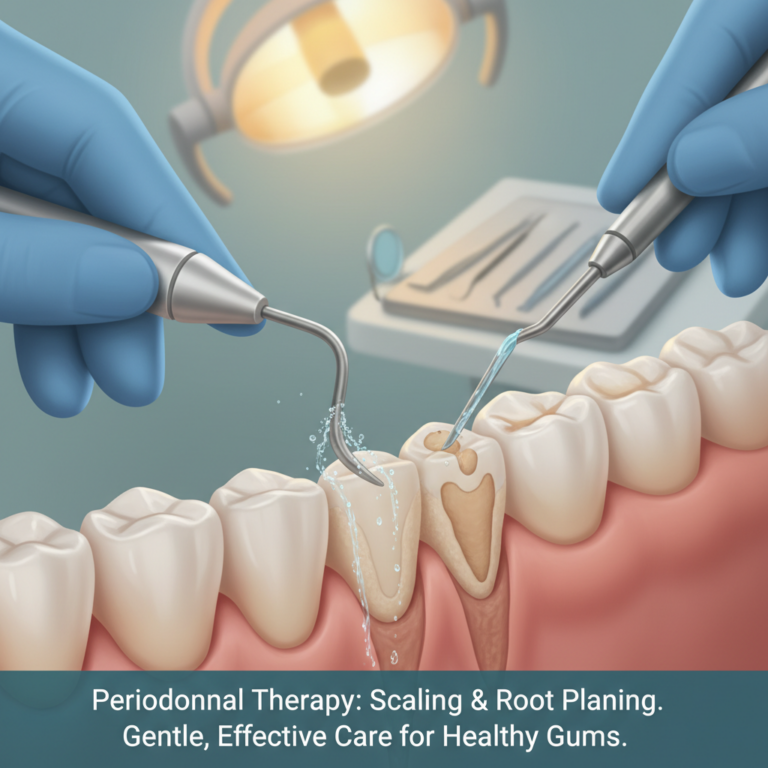
Scaling and root planing: deep cleaning below the gums
Once gum pockets deepen and tartar collects below the gumline, you move beyond the reach of regular cleanings. Scaling and root planing becomes the standard first-line treatment.
According to Cleveland Clinic and the American Academy of Periodontology, scaling and root planing is a deep cleaning done under local anesthesia that:
- Removes plaque and tartar from beneath the gumline
- Smooths the root surfaces to make it harder for bacteria to reattach
- Helps inflamed gums shrink and reattach more closely to tooth roots [3]
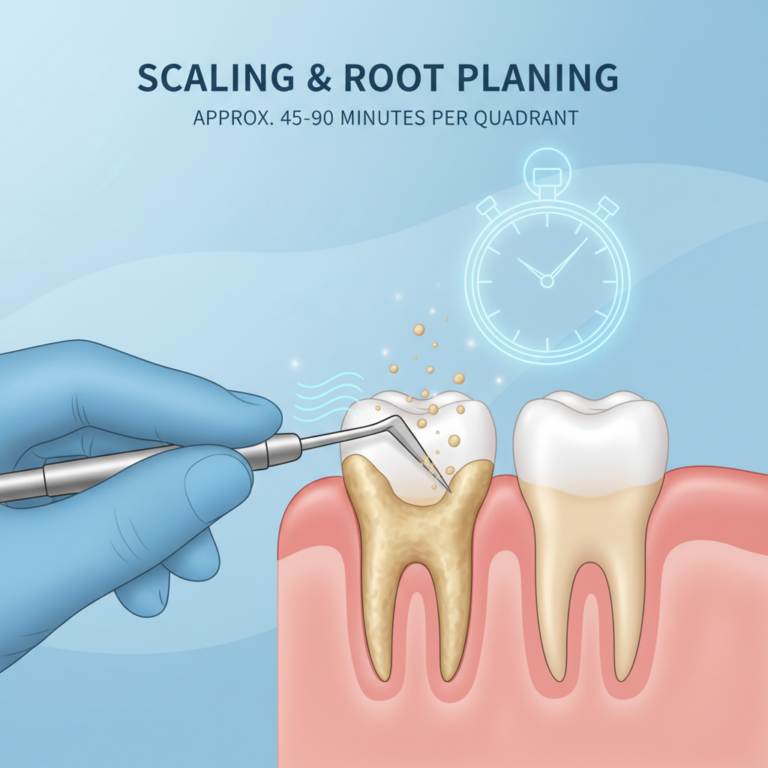
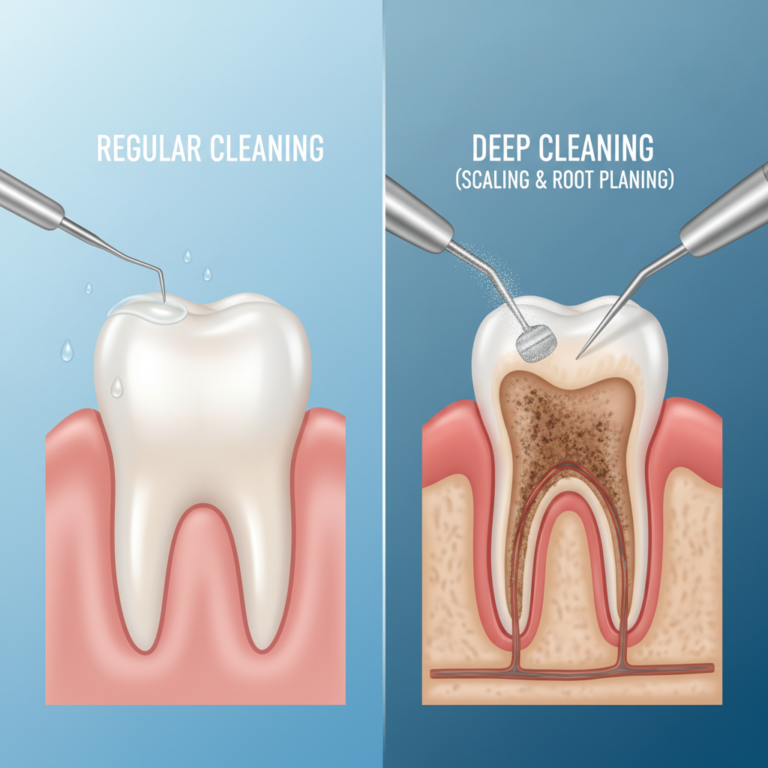
Because this procedure focuses on each root surface in detail, it often takes more time than a standard cleaning and may be spread over two or more visits. If you are trying to understand how these options compare, it can help to read about the difference between regular cleaning and deep cleaning.
Many patients who undergo scaling and root planing do not need additional surgical treatment. However, most will require ongoing periodontal maintenance therapy to keep the disease from returning [4].
If you are wondering about how long you will be in the chair, you can also look into how long does scaling and root planing take so you can plan your appointments appropriately.
Antibiotic and antimicrobial therapies
In moderate and advanced gum disease, bacteria thrive in deep pockets that are difficult to clean mechanically. To help manage this infection, your dentist might recommend:
- Local antibiotics placed directly in the pockets, such as minocycline microspheres (Arestin) or chlorhexidine chips (PerioChip)
- Prescription chlorhexidine mouthwash to reduce bacterial levels
- Tray delivery systems that use custom-fit trays at home to deliver medications under the gums
Cleveland Clinic reports that antibiotics like Arestin and PerioChip can be used alone or along with scaling and root planing by placing them into periodontal pockets to help control infection [5]. Brimhall Dental Group also notes that prescription rinses or slow-release antibiotic chips may be used with surgery to reduce bacterial growth [6].
The American Academy of Periodontology cautions that tray delivery systems are cleared by the FDA only as devices similar to fluoride trays, and that clearance does not confirm the safety or effectiveness of any specific medication placed in them [4]. You should discuss the benefits and limitations of these options with your provider.
Laser periodontal therapy
Some practices use laser technology as part of nonsurgical treatment. Laser therapy uses a small, focused light beam to remove diseased tissue and kill bacteria under the gums.
Cleveland Clinic explains that laser periodontal therapy can remove inflamed tissue and bacteria without cuts or stitches. It can be an alternative to traditional surgery in selected cases, although more severe periodontitis may still require flap surgery [5]. Brimhall Dental Group highlights that lasers can also help gum tissue reattach to teeth and improve overall periodontal health [6].
The American Academy of Periodontology notes that lasers can achieve results comparable to scaling and root planing alone, but they must be used with specific wavelengths and power levels to avoid damaging healthy tissue [4].
Laser therapy is not a universal replacement for deeper surgery, but it can be a helpful adjunct in many treatment plans.
Surgical treatments for advanced periodontitis
If nonsurgical therapy does not fully control your gum disease, or if your periodontitis is severe at the time of diagnosis, your dentist or periodontist may recommend surgery. According to Cleveland Clinic, surgery is typically required for moderate to advanced periodontitis to access deep deposits of tartar, reshape bone, or regenerate lost tissue [5].
Pocket reduction (flap) surgery
Pocket reduction surgery, also called flap surgery, allows your periodontist to fold back the gum tissue and directly visualize and clean deep areas of tartar and infection. The procedure typically involves:
- Lifting the gums away from the teeth
- Removing tartar and diseased tissue from roots
- Smoothing rough bone surfaces if needed
- Repositioning the gums snugly around the teeth
Cleveland Clinic and Brimhall Dental Group both describe pocket reduction surgery as a way to thoroughly clean deep pockets and sometimes reshape bone before suturing the gums back in place [7]. This reduces pocket depth and makes it easier for you and your hygienist to keep these areas clean long term.
Bone grafting and guided tissue regeneration
When periodontitis has destroyed bone around your teeth, regeneration procedures may be recommended to rebuild what was lost. These can include:
- Bone grafting, which places bone or bone-like material in areas where bone has been destroyed
- Guided tissue regeneration, which uses special membranes between bone and gum tissue to encourage regrowth of connective tissue and bone
Cleveland Clinic notes that bone grafting and guided tissue regeneration are used alongside pocket reduction surgery to help rebuild bone lost to gum disease and restore support around teeth [5]. Brimhall Dental Group also lists guided tissue regeneration as a way to help connective tissue regrow after severe gum disease [6].
Newer techniques, including platelet-rich plasma or fibrin applications, can further enhance healing and regeneration in selected cases [1].
Gum grafting for recession
When gums recede due to periodontal disease, tooth roots become exposed and sensitive. This can make your teeth look longer and increase your risk of root cavities. Gum grafting procedures are used to:
- Cover exposed roots
- Reduce sensitivity
- Improve appearance
- Protect roots from further damage
Brimhall Dental Group describes gingival grafting as a surgical treatment that covers exposed roots and can be combined with contouring or pocket reduction to optimize gum shape and health [6].
Complementary home remedies and lifestyle changes
While professional treatment is essential, especially once periodontitis has developed, what you do at home remains a crucial part of how gum disease is treated and kept under control.
Home remedies that support gum health
Certain home methods can help reduce inflammation and bacterial levels, particularly in early gingivitis. These should complement, not replace, professional care:
- Saltwater rinses with sea salt and warm water act as a natural disinfectant and can soothe inflamed gums, according to Wilson House Dental Practice [8]. A 2017 study found that saltwater rinses can reduce plaque similarly to chlorhexidine, although later research suggests they may be less effective than chlorhexidine or some herbal rinses. Prolonged or excessive use can erode enamel due to acidity, so they should be used as directed [9].
- Herbal or natural mouthwashes with ingredients such as lemongrass oil, tea tree oil, sage, guava leaf, or aloe vera have shown promising results in reducing plaque and gingivitis and may serve as useful alternatives or complements to chlorhexidine rinses [9].
- Oil pulling with coconut oil or arimedadi oil mixtures has been shown to significantly reduce plaque and signs of gingivitis in some studies when practiced regularly for 20 to 30 minutes, likely due to reduced harmful oral bacteria and inflammation [9].
- Herbal gels containing ingredients like ginseng or curcumin have demonstrated effectiveness comparable to chlorhexidine gel in reducing plaque and gingivitis symptoms in recent research [9].
These options can help control early gingivitis. However, if you already have deep pockets or bone loss, they will not replace deep cleaning or surgery. Severe pain, heavy bleeding, or loose teeth are signs that you need professional evaluation rather than home care alone [9].
Lifestyle choices that affect your gums
Wilson House Dental Practice emphasizes that lifestyle changes are critical in treating and preventing gum disease. Helpful steps include:
- Quitting smoking or vaping
- Eating a balanced diet rich in fruits, vegetables, lean proteins, and dairy
- Drinking plenty of water
- Controlling systemic conditions like diabetes [8]
The Mayo Clinic also stresses that managing health conditions and stopping tobacco use significantly improves your chances of successful periodontitis treatment [2].
What scaling and root planing feels like
If you have been told you need a deep cleaning, it is natural to wonder whether periodontal therapy is painful and how it compares with your regular visits.
Scaling and root planing is typically performed under local anesthesia, so you should feel pressure and vibration, but not sharp pain. There may be temporary tenderness or sensitivity after the appointments, which usually improves over days to a few weeks as your gums heal and tighten around your teeth.
To get a clearer sense of comfort, healing, and what to expect during and after treatment, you can review is periodontal therapy painful. If you are still deciding whether this step is necessary right now, it may also help to explore do i need a deep cleaning.
Your dentist can explain how many visits you will need, what areas will be treated each time, and what you can do before and after your appointment to minimize discomfort.
Long-term maintenance and prevention
Treating gum disease is only the first step. Periodontitis is a chronic condition, and without ongoing care, it can return and progress again. Many patients who have had scaling and root planing or surgery are placed on a periodontal maintenance schedule, often every three to four months.
Regular maintenance visits allow your hygienist to:
- Clean areas you cannot fully reach at home
- Monitor pocket depths and gum health
- Catch any signs of recurrence early
You can expect your provider to discuss both clinical follow-up and financial considerations. Understanding the cost of deep cleaning vs regular cleaning intent keyword can help you plan for both immediate treatment and ongoing maintenance.
If you are tempted to delay treatment, it is important to understand what happens if gum disease goes untreated. Ignoring the problem can allow infection to destroy bone, loosen teeth, and eventually lead to tooth loss. Untreated gum disease is also associated with higher risks for certain systemic health conditions.
When you treat gum disease early with procedures like scaling and root planing, you are not only protecting your smile today, you are also reducing your risk of tooth loss and more invasive surgery later on.
By partnering with your dentist or periodontist, following through with recommended deep cleanings or surgical procedures, and committing to daily home care, you can control gum disease and support lasting oral health.