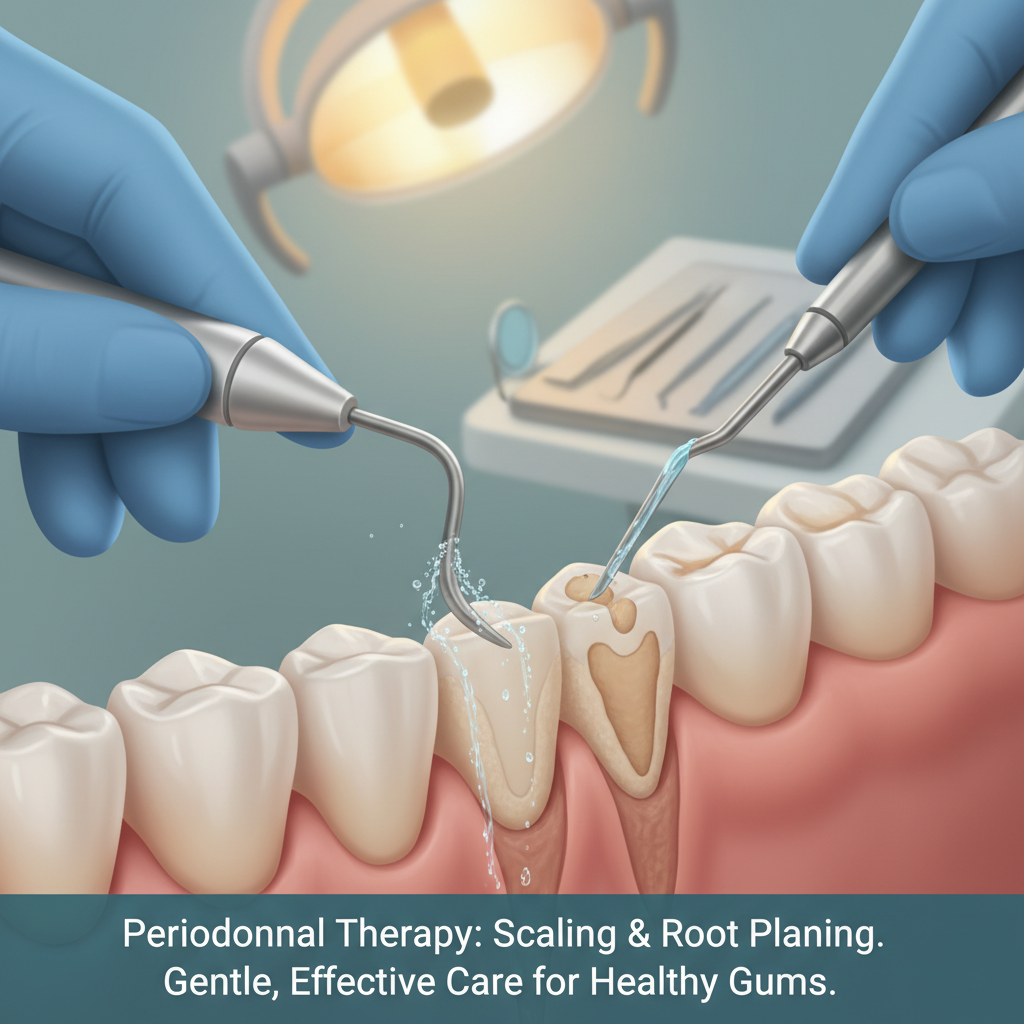
Periodontal therapy often sounds intimidating, especially when you are already worried about bleeding gums, bad breath, or loose teeth. If you are asking yourself, “is periodontal therapy painful?” you are not alone. Many people delay needed care because they are afraid of discomfort, which can unfortunately allow gum disease to progress and make treatment more complex.
Understanding what to expect, how pain is managed, and what you can do to stay comfortable can make a big difference in your experience. Periodontal treatment is not about suffering through procedures. It is about controlling infection, protecting your teeth, and doing so in a way that respects your comfort and anxiety levels.
Understanding periodontal therapy
Periodontal therapy refers to professional treatments that target the supporting structures of your teeth, mainly your gums and the bone underneath. It is used to treat gum disease at different stages and can range from thorough cleanings above the gum line to advanced surgical procedures.
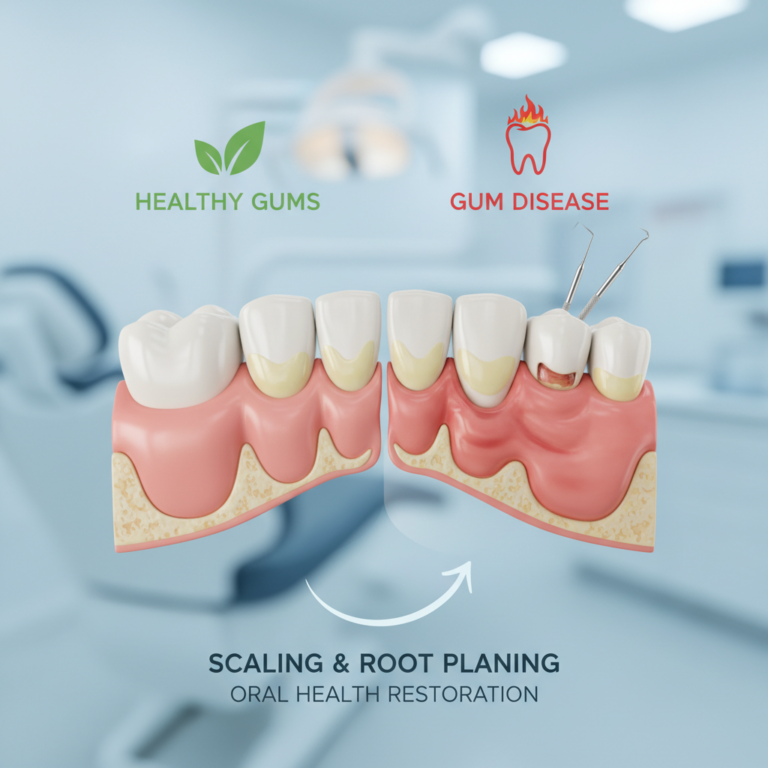
In early gum disease, also called gingivitis, you can often manage the problem with stepped up home care and more frequent professional cleanings. As gum disease progresses into periodontitis, bacteria move deeper under the gums and start to damage the bone that holds your teeth. At this stage, you are more likely to need deep cleaning, also known as scaling and root planing.
If you are not sure where you fall on this spectrum, it can help to look at common signs you need scaling and root planing. Catching issues early often means you can avoid more invasive treatment later.
Early versus advanced gum disease
Early stage gum disease typically shows up as bleeding when you brush or floss, bad breath that does not go away, and mild gum swelling. At this point, treatment may involve:
- Improved brushing and flossing habits
- Antibacterial mouth rinses
- Professional cleanings three or four times a year
These cleanings are similar to your regular checkups and are usually associated with minimal discomfort, if any, when you stay on schedule [1]. You can learn more about options in our guide to early stage gum disease treatment.
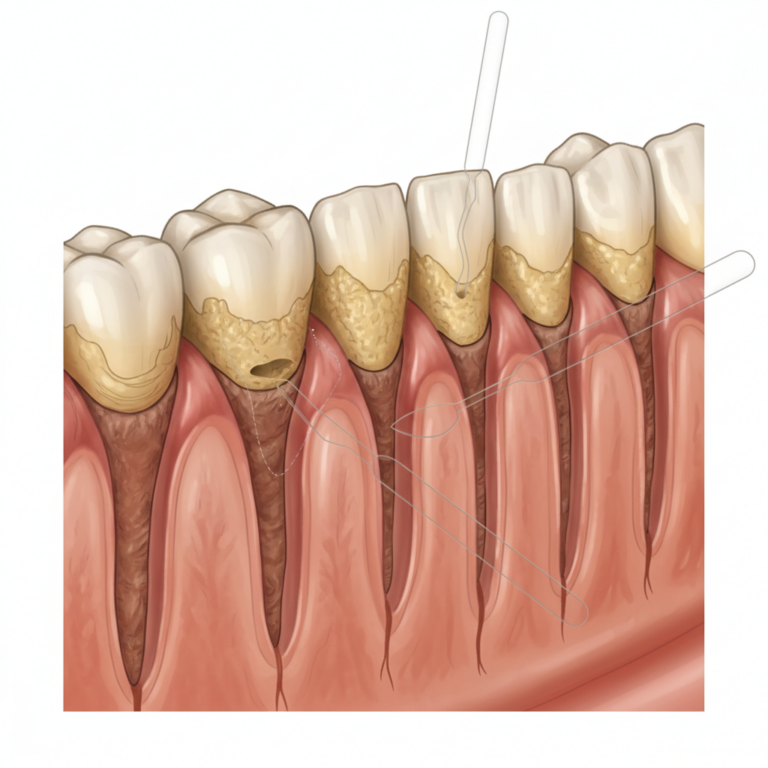
As gum disease advances, pockets form between your gums and teeth. Plaque and tartar collect in these deeper areas where your toothbrush and floss cannot reach. At this point, you move beyond a standard cleaning and into periodontal therapy like scaling and root planing. If the disease continues unchecked, you may eventually need surgical procedures on your gums and bone.
What periodontal treatments might you need?
Not everyone needs the same type of periodontal therapy. What you need depends on how advanced your gum disease is and how your mouth responds to initial treatment.
Non surgical treatments
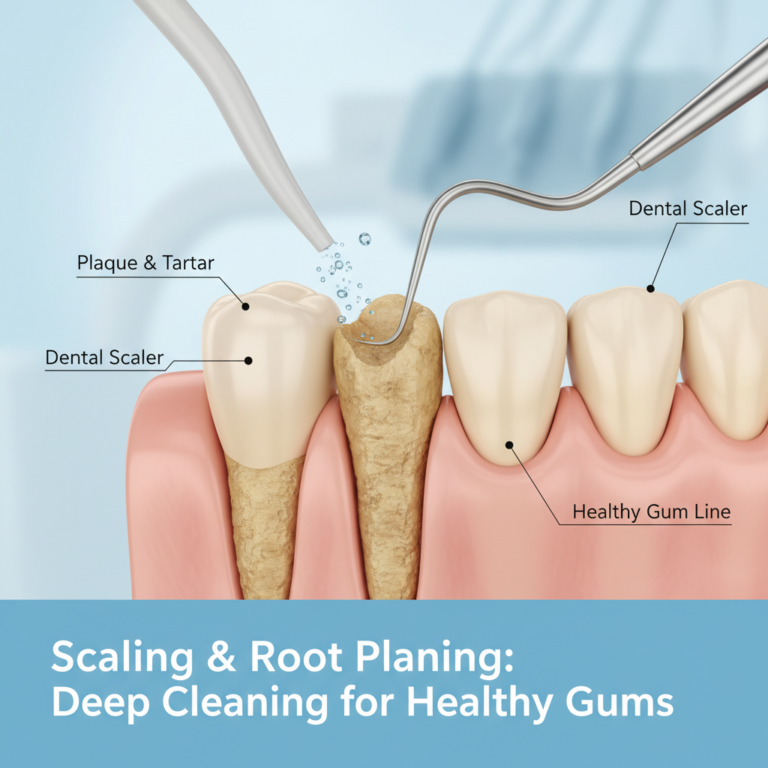
For many people, non surgical care is enough to stop gum disease from progressing. The main non surgical option is scaling and root planing, often called a deep cleaning.
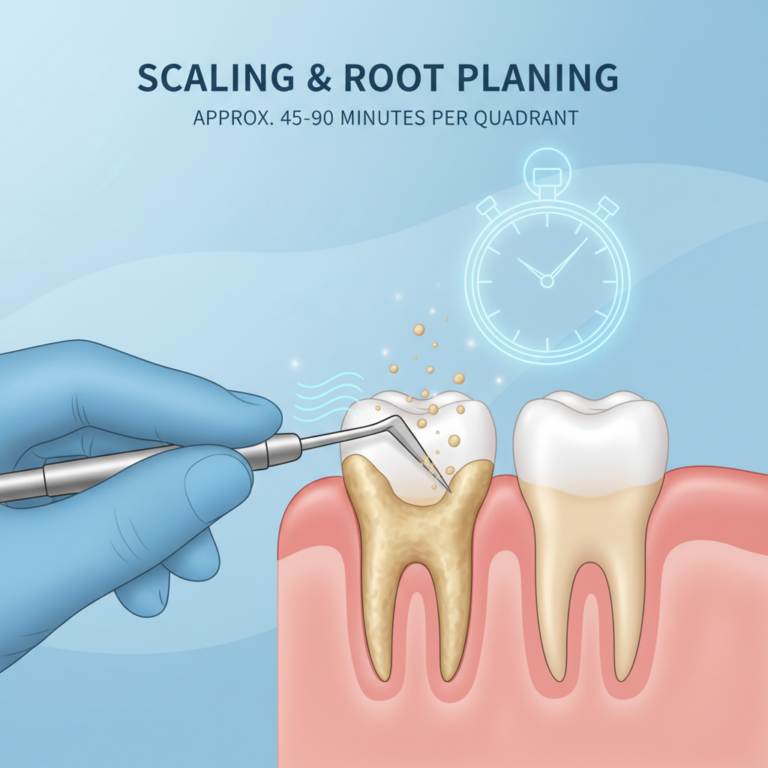
During scaling, your hygienist or dentist removes plaque and tartar from above and below the gum line. Root planing smooths the root surfaces so bacteria have fewer rough places to hide and your gums can reattach more easily.
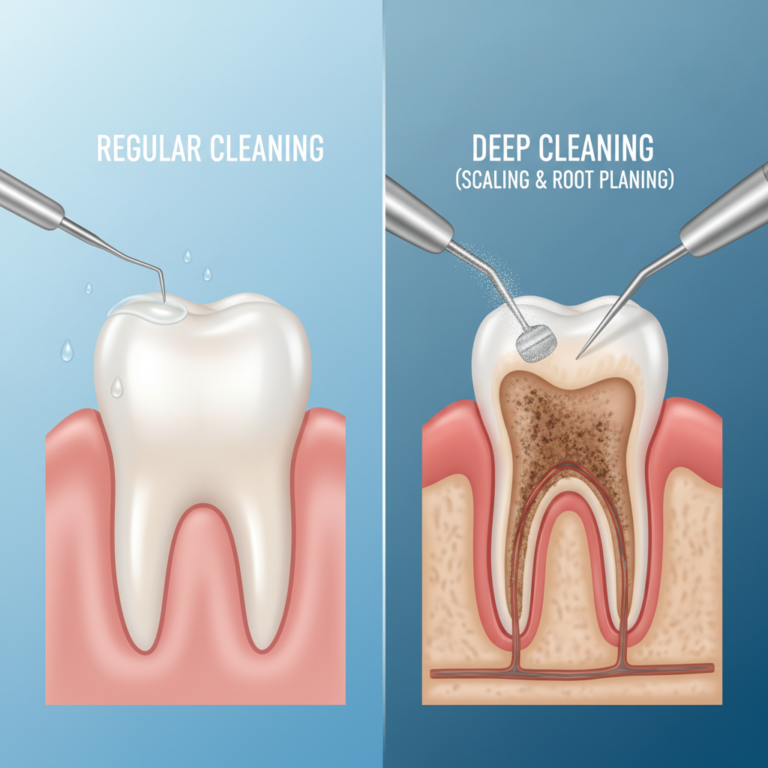
Deep cleaning is different from a standard dental cleaning. If you are comparing the difference between regular cleaning and deep cleaning, the key differences are how far below the gum line the provider works and whether the goal is disease control instead of routine maintenance.
Studies show that scaling and root planing is generally experienced as mildly uncomfortable rather than truly painful, especially when local anesthesia is used. In one study of 218 patients with chronic periodontitis, a little over half reported mild pain in the 48 hours after treatment, not severe pain [2].
Topical anesthetics like gels and creams that contain lidocaine or benzocaine can also be used to numb the gums. A review of periodontal pain control found that these topical options significantly reduced pain during scaling and root planing and performed similarly to injectable anesthesia, especially for people who are nervous about needles [3].
Surgical periodontal treatments
If deep cleaning alone does not control your gum disease, or if your pockets are very deep, your periodontist may recommend surgical options. These can include:
- Flap surgery to clean deep pockets and reduce their depth
- Flap surgery combined with reshaping of the bone around teeth
- Gingivectomy to remove excess or diseased gum tissue
Research comparing postoperative pain in different periodontal procedures found that surgical options, particularly flap surgery with bone reshaping and gingivectomy, caused more pain and sensitivity after treatment than scaling and root planing [4]. All of the surgical techniques caused more tooth sensitivity than nonsurgical deep cleaning in that study.
Even so, these procedures are performed using local anesthesia, and your dentist will prescribe appropriate pain relief afterward. Most people describe the sensation as soreness and tenderness for several days rather than sharp, ongoing pain.
Is periodontal therapy painful during the procedure?
The direct answer to “is periodontal therapy painful during treatment” is that most people experience pressure, vibration, and some sensitivity, but not sharp pain. Modern dentistry uses several techniques to keep you comfortable.
Role of local and topical anesthesia
For scaling and root planing, your dental team will typically numb the areas being treated. This may involve:
- Injectable local anesthesia, similar to what you might receive for a filling
- Topical anesthetic gel applied to the gums, used alone or before an injection
Deep cleaning can feel intense if you were not numb, because the instruments are working below the gum line. When your tissues are numbed with local anesthesia, you should feel pressure and scraping but not pain. Both clinical experience and research support that scaling and root planing is generally well tolerated, especially with anesthesia [5].
Topical anesthetics play a particularly important role for patients with needle anxiety. A systematic review found that gels and creams with agents like lidocaine or benzocaine significantly reduced pain during nonsurgical periodontal therapy and were comparable to injections in many situations [3].
Some offices also use computer controlled anesthetic delivery to administer local anesthesia slowly and at a consistent pressure. This helps decrease the stinging sensation and reduces overall pain perception during injection [3].
Sedation options for anxiety and comfort
If you have significant dental anxiety, simply being numbed may not be enough to help you feel at ease. In those cases, sedation options can be added to your periodontal plan. These can include:
- Nitrous oxide, often called laughing gas, which you breathe through a small nose mask. It helps you feel relaxed within minutes and wears off quickly. Dentists can adjust the dose throughout the procedure, and it is considered a safe and effective way to help you tolerate treatment [6].
- Oral sedation, which involves taking an anti anxiety medication by mouth before your appointment. It usually takes 30 to 60 minutes to work and can provide minimal to moderate sedation without needles, which can be helpful if you are needle averse [6].
These approaches do not replace local anesthesia. Instead, they work with it so that you are both numb and relaxed. Dentists are encouraged to discuss pain and anxiety management options with you so you can receive needed care without unnecessary distress [6].
What to expect after periodontal therapy
Even when a procedure itself is comfortable, it is normal to wonder what the hours and days after treatment will feel like. For periodontal therapy, this often includes temporary soreness, sensitivity, and sometimes mild swelling.
Pain and sensitivity after deep cleaning
After scaling and root planing, it is common to have:
- Tender gums, especially when you touch them or chew
- Mild to moderate sensitivity to cold or hot foods and drinks
- Slight bleeding when you brush or floss near treated areas
In the study of 218 patients who had nonsurgical scaling and root planing, 52.3 percent reported mild pain in the first 48 hours [2]. Nearly half of the patients chose to use pain relievers during that time, most often over the counter options, and dental anxiety was the only factor that clearly predicted who would use more pain medication [2].
Other research on periodontal maintenance visits, which involve probing and cleaning around previously treated gums, found that most people reported low levels of pain. Only about 15 to 33 percent of patients in different studies described their pain as significant, defined as a higher score on a visual analog pain scale [7].
Importantly, dental hygienists were generally able to accurately estimate how much pain their patients were experiencing during these visits, which suggests that your provider can usually tell if you are uncomfortable and respond quickly [8].
Pain after surgical periodontal treatment
If you need surgical gum procedures, you should plan for somewhat more discomfort than after deep cleaning. The study comparing different periodontal treatments found that:
- Flap surgery with bone reshaping and gingivectomy led to significantly higher postoperative pain than scaling and root planing or a more limited flap surgery technique
- All three surgical techniques caused more dentin hypersensitivity, meaning increased response to cold and touch, than nonsurgical deep cleaning [4]
Even so, pain was not described as extreme in most cases, and discomfort tended to decrease as days passed. Your dentist will usually prescribe pain medication, anti inflammatory drugs, and sometimes antibiotics to manage swelling and reduce the risk of infection [1].
Pocket reduction surgery, which is used in more advanced gum disease, is another example. It is done under local anesthesia, so you stay numb during the procedure, and any post surgical pain is typically handled with medication at home [5].
Factors that affect how painful periodontal therapy feels
Not everyone experiences periodontal treatment in the same way. Several factors influence how you perceive pain and how much discomfort you notice.
Level of inflammation and disease severity
More inflamed tissues tend to be more sensitive. Severe periodontal inflammation was associated with higher pain levels after nonsurgical scaling and root planing in the Brazilian study. Patients with more inflamed gums were about 31 percent more likely to report postoperative pain in the adjusted analysis [2].
That finding supports what providers see in practice. When gum disease is treated earlier while inflammation is still moderate, procedures often feel less intense both during and after treatment. This is another reason to address gum problems promptly rather than waiting.
Smoking also appears to increase postoperative discomfort. Smokers in the same study had a higher likelihood of pain after deep cleaning than nonsmokers, even after accounting for age, gender, and anxiety levels [2].
Dental anxiety and pain perception
Your mindset going into periodontal therapy matters. Anxiety and anticipated pain can heighten your perception of actual discomfort. Multiple studies have shown that:
- Patients with higher dental anxiety scores tend to report more pain during and after periodontal therapy, including scaling and root planing and maintenance visits [9]
- Anxiety before treatment correlates with both how much pain you expect and how much you actually feel [3]
Some research suggests that just one or two questions about dental anxiety can help identify patients who are likely to experience more pain, so providers can plan additional pain control measures [8]. Sharing your fears openly with your dentist or hygienist is not complaining. It gives them critical information to tailor your care.
Individual tolerance and age
Pain tolerance varies widely from person to person. Age also seems to play a role. In the study that compared surgical and nonsurgical periodontal treatments, pain and discomfort generally decreased with increasing age. In other words, older patients tended to report less pain across all types of periodontal therapy [4].
On the other hand, in a smaller maintenance treatment study, age was not strongly linked with pain experience, which suggests that individual differences may matter more than age alone [10]. Either way, your provider will not assume how you feel. They will rely on your feedback and their clinical observation.
How dentists manage pain during periodontal therapy
Modern periodontal care includes a full toolkit for managing pain and discomfort. These methods work together to help you stay as comfortable as possible.
Anesthetic and medication strategies
During and after treatment, your dental team may use a combination of:
- Topical anesthetic gels or creams placed on your gums before or instead of injections
- Local anesthetic injections to numb the areas being treated
- Computer controlled anesthetic delivery systems to reduce the sting of injections [3]
- Preemptive anti inflammatory medications taken before surgery to lessen pain afterward
- Postoperative nonsteroidal anti inflammatory drugs and sometimes steroids to reduce swelling and pain, used for a limited period to avoid side effects [3]
Antibiotics may also be prescribed after certain procedures to control infection, which indirectly reduces pain by helping tissues heal more smoothly [1].
Non surgical comfort options
For some types of periodontal therapy, especially in earlier stages, there are less invasive options that can further limit pain:
- Tray periodontal therapy uses custom made trays that hold medication under your gums for short periods each day. At first, the trays might cause slight soreness, but they are designed to fit comfortably overall [1].
- Laser gum treatment uses concentrated light to remove bacteria and inflamed tissue. It often requires only minimal anesthesia and usually results in less discomfort and faster healing than traditional methods [11].
Scaling and root planing itself is generally considered to be on the lower end of the pain scale, particularly when topical or local anesthesia is used. Some patients notice only mild soreness and sensitivity afterward, which can be managed with over the counter pain relievers and gentle care [5].
What you can do to minimize discomfort
You play an active role in how comfortable your periodontal therapy feels, both by the questions you ask and the habits you follow.
Before your appointment
Before you start periodontal treatment, consider:
- Asking your dentist to explain exactly what to expect during and after each step. Knowing what is coming often reduces anxiety.
- Sharing any past negative dental experiences so your provider can adjust their approach.
- Discussing sedation options such as nitrous oxide or oral anti anxiety medication if you feel very nervous.
- Reviewing your medical history and any medications you take, since these can impact anesthetic choices.
You can also ask how long your visits are likely to take. Many people find it helpful to understand how long scaling and root planing takes so they can plan their day and bring any comfort items they may want.
After your appointment
Once treatment is complete, follow the home care instructions you receive. These often include:
- Taking prescribed or recommended pain medication before numbness fully wears off
- Rinsing gently with warm salt water to soothe the gums
- Eating soft, cool foods for the first day or two
- Brushing and flossing carefully but consistently to keep the area clean without traumatizing the tissues
Relaxation techniques like deep breathing can also help. Beyond lowering anxiety, these practices may reduce your overall perception of pain during the healing period [5].
If discomfort feels stronger than expected, or if you notice increased swelling or bleeding, contact your dentist. It is better to ask for help early than to wait and worry.
Why early periodontal care hurts less in the long run
Putting off periodontal treatment because you are afraid of pain can have the opposite effect of what you want. The longer gum disease is left untreated, the more likely you are to need more intensive procedures and to experience greater discomfort.
Early intervention with deep cleaning and careful maintenance often prevents the need for surgery and helps you keep your natural teeth. If you are wondering do I need a deep cleaning, or if you are trying to understand how gum disease is treated and what happens if gum disease goes untreated, it is worth speaking with a dentist soon instead of waiting until you are in pain.
You may also find it helpful to understand the practical side, including the cost of deep cleaning vs regular cleaning and whether gum disease can be reversed. Knowing the clinical facts and the financial picture together can make the decision to move forward with care feel more manageable.
Periodontal therapy is not about forcing yourself through pain. It is about partnering with your dental team to control infection, protect your teeth, and keep you as comfortable as possible at every step.
If you are noticing bleeding gums, persistent bad breath, or gum recession, taking action now is usually the most comfortable and effective choice. With modern anesthetics, thoughtful pain management, and open communication about your anxiety and goals, periodontal therapy does not have to be something you fear.